Chronic enteropathy – a complex topic which raises many questions. The number of patients being presented with “chronic diarrhoea” seems to be increasing. This article will look at frequently asked questions.
As part of our expert panels, Laboklin regularly invites specialists to discuss a range of fascinating topics. We have compiled some interesting answers from the expert panel on the topic of chronic enteropathy.
The participants were: Prof. Stefan Unterer, Head of the Clinic for Small Animal Medicine at the Vetsuisse faculty of the University of Zurich, a well-known gastroenterologist. Dr Silke Salavati-Schmitz teaches at the Royal Dick School in Edinburgh, UK, and is known for her work on the gut microbiota and the use of probiotics. As an expert in dietetics, PD Dr Petra Kölle from the Clinic of Small Animal Medicine of the LMU Munich were able to provide valuable information on the topic of nutrition for patients with chronic diarrhoea. Prof. Wolfgang Bäumer, Head of Veterinary Pharmacology and Toxicology at the FU Berlin, highlighted the subject of treatment with a focus on pharmaceutical legislation. Important aspects on the histopathological examination of intestinal biopsies were contributed by PD Dr Heike Aupperle-Lellbach, pathologist and scientist at Laboklin.
The question of terminology – What is the current definition of “chronic enteropathy”?
Dr Silke Salavati-Schmitz’s first answer is pragmatic: Actually, there is none! Chronic enteropathy is rather used as an umbrella term. Currently, it is almost used as a synonym for the term IBD, which was previously limited to steroid-responsive intestinal diseases. It is then subdivided into food-responsive (most of them) and steroid-responsive. Whether the group of antibiotic-responsive enteropathies should still be referred to as such is debatable. It is surprisingly small if treatment is carried out according to more recent criteria.
-
Fig. 1: Faeces of a dog with chronic enteropathy
Photo credits: Dr Jennifer von Luckner
-
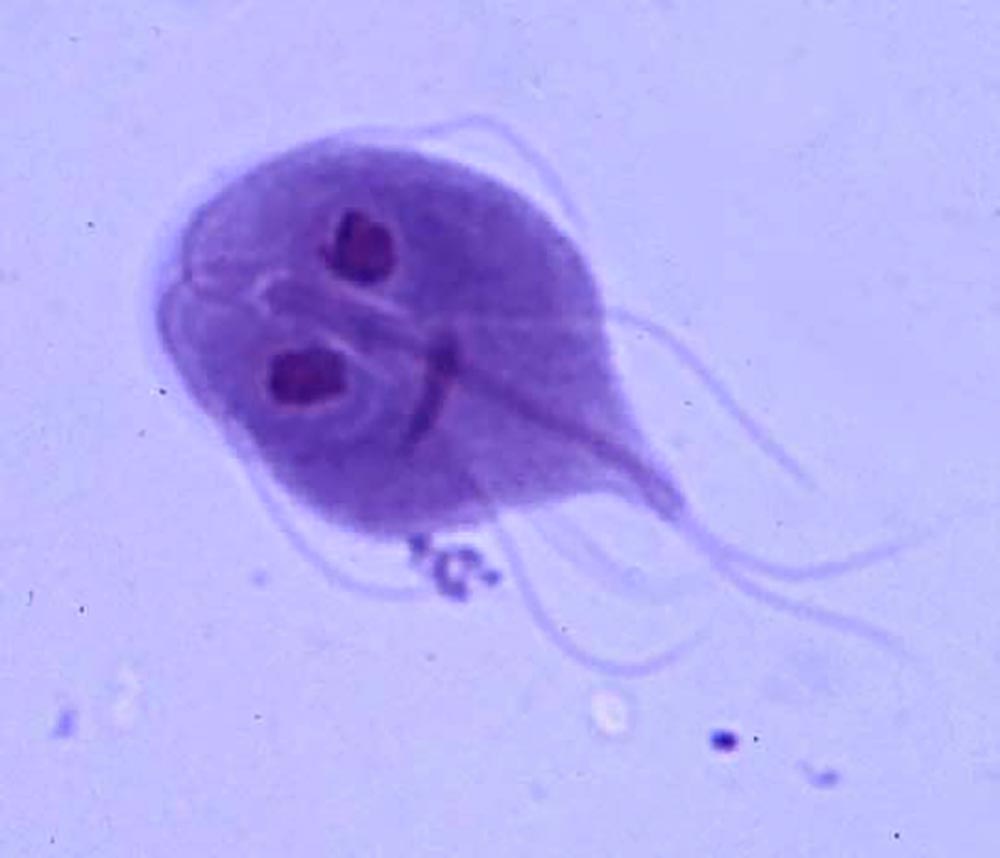
Fig. 2: Close-up of Giardia spp.
Photo credits: Laboklin
Diagnosis
How often does it happen that patients with chronic enteropathy do not have any abnormal blood parameters?
Dr Silke Salavati-Schmitz reports that this is not unusual at all. There may be no evidence of inflammation (e. g. leukocytosis, elevated CRP levels) and/or malabsorption (e. g. decreased serum folic acid or cobalamin levels), but this does not rule out enteropathy. And clinically, too, it can sometimes not be that simple. Not every patient suffering from intestinal disease also has diarrhoea (Fig. 1). Some only lose weight or have vomitus, others only experience behavioural changes.
How important is the faecal analysis?
The experts agree that a faecal analysis for parasites is a must. Even if Giardia is detected, it cannot always be simply interpreted as the cause of diarrhoea. Bacteriological examinations for pathogenic agents are only useful if pathogens
(e. g. Salmonella) are suspected to be the causative agent and/or should be excluded. In general, antibiotics should not be given without a specific indication, simply because of microbiological findings in the faeces.
How relevant is a positive result for Giardia in a dog with chronic diarrhoea?
Prof. Stefan Unterer and Dr Silke Salavati-Schmitz start to ponder. An exact answer cannot be
given as data is lacking. In some cases, Giardia (Fig. 2) probably colonise secondarily in a diseased intestine, or they are an incidental finding. Maybe they are just commensals. Since there is currently no way to distinguish whether or not Giardia are responsible for the signs and symptoms, treatment with fenbendazole is routinely given and it is recommended to follow hygiene measures.
Are endoscopy and biopsy always necessary?
Prof. Stefan Unterer agrees with Dr Silke Salavati-Schmitz: For cats, rather yes, as a distinction between inflammation and low-grade malignant lymphoma can only be made by histopathological examination of intestinal biopsies. In dogs, it is not so much of an issue as there is usually infiltration with lymphocytes and plasma cells, and intestinal neoplasms are rare. However, if treatment fails, appropriate diagnostic measures can clarify differential diagnoses such as ulcerative colitis, protothecosis and eosinophilic enteropathy, which require a different or more aggressive therapeutic approach. In unclear cases, intestinal biopsies should be considered before starting long-term steroid treatment. Both experts emphasise that it is always useful to take biopsies when performing an endoscopy. The macroscopic appearance of the intestine is never pathognomonic for a specific disease. Likewise, a normal appearance of the intestinal mucosa does not exclude a pathological condition.
Are endoscopic biopsies sufficient or is it better to have surgical full-thickness biopsies?
PD Dr Heike Aupperle-Lellbach points out that some criteria of IBD, such as villous atrophy, are not easy to assess by looking at superficial biopsies of the small intestine. For protein-losing enteropathy, she also prefers a full-thickness biopsy for a complete evaluation, as far as it can be clinically justified (wound healing disorders in protein deficiency). The diagnosis of lymphoma can usually be made from endoscopic biopsies, provided that the affected section of the intestine was reached and sampled.
What about pre-treatment with immunosuppressants before taking a biopsy?
Dr Silke Salavati-Schmitz is concerned that this can reduce inflammatory reactions and make it more difficult to differentiate the lymphoma. She recommends a minimum of two weeks between medication and sampling, if possible. PD Dr Heike Aupperle-Lellbach comments that from the pathologist’s point of view, if the lymphoma is extensive, there is a good chance that it can still be diagnosed. However, when planning full-thickness biopsies, it should be kept in mind that the administration of glucocorticoids may increase the risk of intestinal suture dehiscence.
Serum cobalamin levels are used to assess malabsorption, and its substitution is part of the treatment to restore gut health. But what significance do low levels of serum folic acid have?
Prof. Stefan Unterer confirms that low levels of serum folic acid also indicate intestinal absorption disorders. So far, a prognostic relevance could not be proven and it is unclear to what extent folate substitution is necessary in dogs with chronic enteropathy. Nonetheless, it is recommended.
What is the informative value/significance of calprotectin as biomarker?
Calprotectin indicates inflammatory processes and is elevated in the faeces of dogs with chronic enteropathy. The level of faecal calprotectin correlates with the severity of enteropathy. Additionally, in one study, higher levels were found in dogs with steroid-responsive enteropathy (as opposed to those that did not require steroids), which can potentially guide treatment decisions. However, Dr Silke Salavati-Schmitz points out that the amount of calprotectin in the faeces of small animals with chronic intestinal diseases is often not as high as, for example, in people with Crohn’s disease (where calprotectin is used as a marker of improvement or remission), so that many values fall into the “grey area”. The reason for this could be that calprotectin mainly comes from neutrophil granulocytes, whereas in dogs there is often lymphoplasmacytic, eosinophilic or “mixed” inflammation.
The microbiome
A dysbiosis analysis is carried out by looking at bacterial markers which give an impression of the functional groups in the intestine. Their balance is important for a healthy intestinal environment. A score is calculated from the levels of different key bacteria. Which key bacteria are involved?
Typical bacterial markers are, for example, Clostridium hiranonis or Faecalibacterium prausnitzii. The former converts primary to secondary bile acids, the latter produces short-chain fatty acids. These substances have important functions in the intestine such as providing energy for intestinal epithelia, reducing inflammatory reactions or promoting the repair of intestinal mucosa. Based on an algorithm, a score or index is determined from 6 – 9 different key bacteria.
How often is the score/are the markers affected in chronic enteropathy?
Experience shows that most dogs with chronic enteropathies have a dysbiosis. However, Dr Silke Salavati-Schmitz emphasises that dysbiosis can also be present in many other acute and chronic diseases both within and outside the gastrointestinal tract. Thus, it is not really a good diagnostic marker for the presence of chronic enteropathy, but it does provide an indication of a change in the microbiota, which can be of therapeutic value.
Treatment
What about a standard treatment plan that can be adopted for all patients with chronic enteropathy?
Certainly, the regimen is always similar. Start with a diet, usually in combination with pre- and probiotics, then use immunosuppressants. PD Dr Petra Kölle reports that the response to diet and pro-/prebiotics can be highly individual. It is very important to her that patients are not immediately classified as treatment failure if the first dietary attempt is not successful. Often, several approaches are necessary. If there is any doubt, a home-made diet should definitely be tried. In food counselling, it can sometimes be observed that a home-made diet such as horse + potato is tolerated, but canned horse + potato is not.
For how long should you follow a diagnostic elimination diet?
In contrast to dermatology, PD Dr Petra Kölle confirms that in gastroenterology 3 weeks are usually sufficient to assess whether or not there is an improvement due to the change in diet.
When is it possible to change back to the regular diet?
If clinical signs improve after changing the diet, it should be fed exclusively for a longer period of time. It is assumed that this period is at least 3 months. However, one study showed that most dogs that were changed back to their original or another “normal” diet after a certain period of time suffered a relapse within a year.
On the subject of probiotics: Which products do the experts prefer?
Dr Silke Salavati-Schmitz considers Enterococcus faecium, contained in many veterinary-approved products, to be a good choice for acute problems, such as stress-induced colitis, and as an adjuvant therapy for infectious diseases (e. g. Tritrichomonas foetus in cats). For chronic diseases, on the other hand, probiotic mixtures are usually used. The most reliable data is currently available for VSL#3 (Vivomixx® in Europe, Visbiome® in the USA).
What is the opinion about food with added probiotics?
Probiotics are live microorganisms which can have a health-promoting effect when ingested orally in sufficient quantities. Prof. Wolfgang Bäumer points out that only Enterococcus faecium is approved for being mixed into animal feed in the EU. It is difficult to assess whether supplementing the feed with this one bacterium is enough, whether its concentration is sufficiently high and, last but not least, whether it is still viable in the feed.
When should/can antibiotics be used?
Prof. Unterer and Dr Salavati-Schmitz agree that, nowadays, using antibiotics is a last resort and should only be done when absolutely necessary. This is the case if there is bacterial infiltration or if the patient suffers from a gastrointestinal disease and shows signs of a systemic inflammatory reaction. Antibiotics should definitely no longer be used as long-term medication.
Dr Jennifer von Luckner
Further Reading:
-
Jergens AE, Heilmann RM. Canine chronic enteropathy – Current state-of-the-art and emerging concepts. Front Vet Sci. 2022 Sep 21;9:923013.
-
Ewald N, Rödler F, Heilmann RM. Chronische Enteropathien bei der Katze – diagnostische und therapeutische Aspekte. Tierarztl Prax Ausg K Kleintiere Heimtiere 2021; 49(05): 363-376.