Introduction
The pancreas fulfils multiple vital metabolic functions. The exocrine pancreas secretes digestive enzymes and is therefore essential for the utilisation of nutritional components.
Inflammatory and degenerative diseases of the exocrine pancreas are important in cats and dogs.
The following text provides an overview of exocrine pancreatic diseases as well as how to diagnose them.
Pancreatitis in general
Pancreatitis can be acute or chronic. Whereas acute forms are associated with severe clinical symptoms, chronic forms can be clinically unremarkable.
The differentiation between acute and chronic forms is based on the organ damage present, which can only be determined histologically.
The digestive enzymes are generally produced as inactive proenzymes in order to protect the organ tissues against autodigestion. Damage of the pancreatic tissue leads to an increased release of enzymes. As a result, pancreatic tissue and adjacent adipose tissues are destroyed.
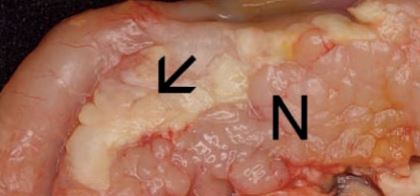
- Fig. 1: Acute pancreatic necrosis (arrow) next to macroscopically normal pancreatic tissue (N) in a cat
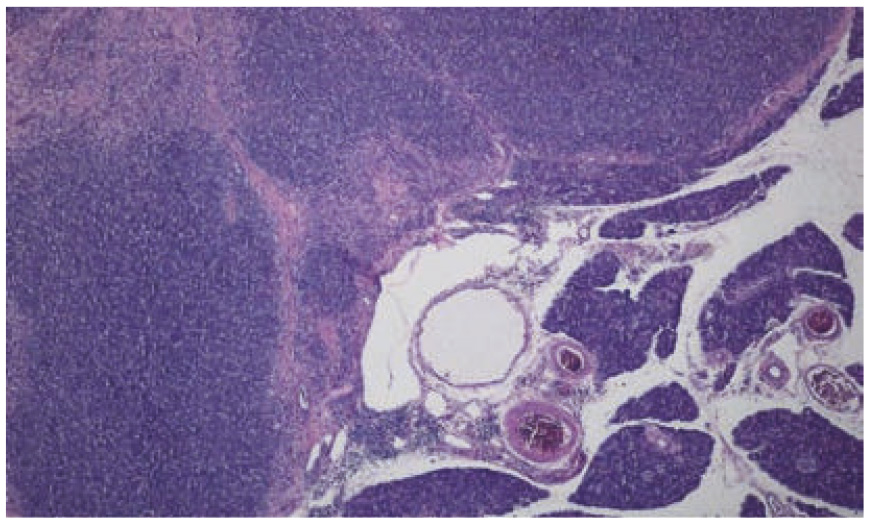
- Fig. 2: Well differentiated feline pancreatic carcinoma.
Tissue necrosis is the dominant finding in peracute cases, whereas no inflammation is detectable histologically (yet). Therefore it is often more correct to speak of acute pancreatic necrosis in these cases, rather than pancreatitis.
In acute pancreatitis there is inflammatory cell infiltration dominated by neutrophilic granulocytes with necrosis. Necrosis of the peripancreatic adipose tissue appears as rough white papules which often mineralize due to inclusion of calcium salts.
In chronic pancreatitis, a lymphoplasmacellular inflammation is predominantly found. Additionally atrophy of the pancreatic parenchyma with subsequent fibrosis and pancreatic cirrhosis may develop.
Acute Pancreatitis/Acute Pancreatic Necrosis
Acute pancreatitis is a lifethreatening syndrome found more often in cats than in dogs. (Fig. 1)
In cats, acute pancreatitis often occurs in combination with (cholangio) hepatitis and/or enteritis, whereas the isolated forms are more common in dogs.
The cause is often unclear, although a multifactorial genesis is assumed: obesity, lack of exercise and a high fat diet, certain drugs (e.g. sulfonamides, azathioprine, glucocorticoids), trauma (e.g. during abdominal surgical procedures), or systemic infections (e.g. feline toxoplasmosis).
The clinical symptoms are unspecific and vary in their severity. Typical signs include anorexia, vomitus, diarrhoea, and abdominal pain. Additional fever, tachypnoea or even shock can also be seen.
Because of these unspecific clinical symptoms, specific indirect test methods are necessary to quickly and confidently reach a diagnosis.
Primarily serological tests are crucial to the diagnosis (see below).
Depending on the severity of the inflammation and necrosis, full recovery of the pancreatic function is possible or partial tissue necrosis with subsequent fibrosis if the animal survives the disease.
Chronic Pancreatitis and Exocrine Pancreatic Insufficiency (EPI)
The chronic form of pancreatitis can develop from a recurrent acute inflammatory pancreatitis or from a silent progressing interstitial pancreatitis. In the recurrent form, which is more common in dogs, clinical phases with indigestion occur repeatedly with intermittent vomiting and diarrhoea. Symptoms are usually selflimiting and less severe than in cases of acute pancreatitis.
Laboratory values can be altered as in cases of acute pancreatitis, but may be within normal range. Between the episodes with clinical symptoms, the dogs show no abnormalities and so the indigestion is in many cases not associated with a pancreatitis.
If a major portion of the functional pancreas tissue is atrophic or has been replaced with connective tissue the animal develops an exocrine pancreas insufficiency due to the inadequate production digestive enzymes. Clinically, these animals develop chronic diarrhoea with large amounts of faeces and steatorrhoea. The animals lose weight despite a consistent appetite.
In general no morphological changes of the pancreas are visible using diagnostic imaging techniques, so again it is necessary to use indirect test methods to diagnose “Exocrine Pancreatic Insufficiency”.
Nodular Hyperplasia
Nodular hyperplasia of the exocrine pancreas is relatively common in older dogs and cats.
Clinically, these are without relevance and are mostly incidental findings during laparotomy. Nodular hyperplasia is generally found as multiple small nodules dispersed within the pancreatic parenchyma. Histologically, the nodules consist of non encapsulated foci of partly hyperplastic, partly normal acini.
Feline pancreatic islet amyloidosis must be considered as differential diagnosis in cats.
Tumours of the Exocrine Pancreas
Tumours of the exocrine pancreas are relatively rare in dogs and cats.
(Benign) pancreatic adenomas are extremely rare, and their distinction from nodular hyperplasia can be difficult, even histologically, but is barely of clinical relevance.
Generally, pancreatic carcinomas can arise from the excretory ducts or the acini. Whereas ductal tumours are most common in humans, acinar tumours are more likely to develop in dogs and cats. These present as single or multiple masses within the pancreas, with infiltrative growth and an early tendency to metastasis (particularly into the liver, lymph nodes, intestine, lung, peritoneum), so that at the time of diagnosis most have already metastasized. (Fig. 2)
Diagnosis of Pancreatic Disease
Serum lipase and serum amylase
Both enzymes are elevated in serum from patients with pancreatitis and pancreatic necrosis. However, the values are only significant if they are more than three times as high as the upper reference range.
False positive and false negative results are common, especially in cats, since lipase and amylase can also be elevated due to disease processes in other organ systems (e.g. hepatopathies, kidney failure) and in the contrary significant elevations may be missing.
Pancreatic Lipase (cPLI, fPLI)
Detection of pancreatic lipase immune reactivity is very specific and much more sensitive. PLI is species specific and is found only in the pancreas.
Until recently, PLI detection was difficult due to the fact that detection could only be carried out in a patented laboratory in the USA.
LABOKLIN has recently established a validated test for the detection of PLI that is comparable to the one used in the USA. Thus, the PLI test results are now available fast and without additional shipping costs.
Trypsin-like Immunoreactivity (cTLI, fTLI)
cTLI or fTLI should be considered the most important values for the detection of pancreatic insufficiency. In this test, both trypsin and its proenzyme, trypsinogen, are detected in serum.
In cases of EPI, these values are considerably decreased.
A significant elevated TLI value is, on the other hand, indicative of a pancreatitis. It is however, critical for the result interpretation that the animal was fasted before blood sampling. TLI can also be significantly increased in cases of renal failure, especially in cats, so the renal parameters should additionally be determined.
Pancreatic Biopsy – Histology
Significantly more difficult is the surgical collection of a pancreatic biopsy for histopathology. If a representative localisation is submitted, the type and degree of the pancreatic damage can be made.
Since a patient with acute pancreatitis has a significantly increased risk of anaesthesia, histopathology plays a rather minor role in such cases.
However, if a laparotomy is performed in order to diagnose intestinal problems of unknown aetiology, pancreatic samples should be collected, together with transmural gastric, intestinal, lymph node and hepatic biopsies in order to obtain a full picture and to diagnose chronic changes.
Histopathology is, however, necessary in order to diagnose pancreatic neoplasia.
Conclusions
The diagnosis of exocrine pancreatic diseases can be quite a challenge for the clinician as most animals do not show any specific symptoms. Serological testing is of crucial importance and, if necessary, collection of biopsies.
Table: Laboratory Parameters of the Exocrine Pancreas – Guidelines
| Lipase | Amylase | TLI | PLI | |
| Normal values | Dog: < 300 Cat: < 280 |
Dog: < 1650 Cat: < 1850 |
Dog: > 5 < 50 Cat: > 12 < 82 |
Dog: < 200 Cat: < 3,5 |
| Pancreatitis | Variable, generally increased | Variable, generally increased | Dog: > 50 Cat: > 100 |
Dog: > 400 Cat: > 5,4 |
| Exocrine pancreatic insufficiency (EPI) | Variable | Variable | Dag: < 2,5 Cat: < 8 |
Variable |