There are many methods available for the detection of infectious diseases in animals. It is important to differentiate between detection of the infectious agent (= direct detection of infection) and the detection of antibodies (= indirect detection of infection). Various methods can lead to different results. In many cases, a combination of tests may be useful, especially since no test has 100% sensitivity and specificity.
Antibody detection
There are several reasons that serum antibodies can be present, and antibody detection methods are generally not able to distinguish between a reaction to vaccination, infection, or maternal antibodies. Puppies and kittens can retain maternal antibodies up to 16 weeks of age. This should be considered in positive animals depending on their age. Antibodies are also not produced directly following infection. Antibodies may therefore not be detectable in cases with peracute or acute disease. In cases of acute infections, a 4-fold increase in titre may be detectable in paired serum samples collected 2-4 weeks apart, if the animal has not been vaccinated in between times.
Pathogen detection
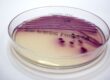
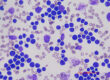
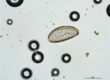
The choice of the right sample material is especially important for good diagnostics in direct pathogen detection, and depends on where the pathogen can be expected at the time of sampling (e.g. in the blood or the mucous membranes). The prerequisite is knowing how the pathogen spreads in the body and how it is shed in the environment. Sampling is best done before treatment begins, in order to avoid possible false negative results. For molecular diagnostics via PCR (polymerase chain reaction), it is important to remember that e.g. if live vaccines are used, these can be found in sample material for several weeks after application and can cause false positive results. In general, a positive result shows that a pathogen is present in the sample material and therefore is usually equivalent with an infection. A negative result, on the other hand, does not rule out an infection.
Kennel cough – a multifactorial disease
The canine respiratory disease known as kennel cough (canine infectious tracheobronchitis) is characterized by an acute, extremely harsh and hacking cough.
Viral pathogens, including canine adenovirus type 2 (CAV-2) and canine parainfluenza virus (CPiV) are the most important causes. Influenza viruses, canine distemper virus, canine herpesvirus (CHV) and canine respiratory coronavirus (CRCoV) are less common causes. Primary bacterial pathogens include Bordetella bronchiseptica. Once the respiratory epithelium has been damaged by one or more of these pathogens, other bacteria and mycoplasma can also be causes of severe respiratory disease. E. coli, Pasturella, streptococci, Pseudomonas, and Klebsiella are particularly common.
The initial diagnosis is based on the history (sudden onset of clinical signs, possible exposure to other dogs, not vaccinated, etc.) and the clinical signs.
Multiple pathogens can be detected by PCR, ideally on dry nasal and/or oral swabs or bronchoalveolar lavages, especially at the beginning of the disease. In order to use the speed and sensitivity of the methods to best advantage, it is best to include PCRs for bacterial components such as Bordetella bronchiseptica. It is, however, important to note that it is not possible to obtain an antibiogram based on a PCR. Mycoplasma require special selective media and grow very slowly, so that PCR is also the method of choice for their detection.
Since bacteria are primarily responsible for severe courses of disease, culture of deep oral swabs or tracheal or bronchoalveolar lavages followed by an antibiogram are always especially important in animals with signs other than an unproductive cough with no additional signs of disease.
The detection of antibodies is less useful, since the pathogens involved are widely disseminated in the canine population. It is also not possible to distinguish between antibodies acquired following vaccination, and those acquired following infection (important e.g. for CAV-2, CPiV, and CDV as core vaccines). Only detection of antibodies in paired serum samples can provide information on the presence of an infection, and then generally only in retrospect. Because they can cause latent infections, anti CHV antibody titres sink rapidly following infection and are therefore only conditionally recommended for detection of infection.
Feline respiratory disease complex
Feline respiratory disease complex is a common name for an infectious disease of the respiratory tract and mucous membranes of cats. It is a complex of clinical signs of disease that can be caused by a variety of pathogens and that affect the nose, oral cavity, and eyes. The clinical signs are very variable and therefore cannot generally be clearly attributed to a specific pathogen. They range from mild, serous nasal discharge to deadly systemic disease. Animals develop a cold, conjunctivitis, oral lesions, fever, and pneumonia.
Feline calicivirus (FCV) and feline herpesvirus 1 (FHV-1) are involved in most cases of feline respiratory disease complex. Chlamydia felis, mycoplasma, and Bordetella bronchiseptica are among the primary bacterial pathogens that can be involved. Unspecific bacteria are often also involved as secondary pathogens. As in the case of kennel cough, feline respiratory disease complex is routinely diagnosed via PCR from dry swabs (conjunctiva, oral cavity and/or pharynx). Since chlamydia are intracellular, they cannot be detected using normal bacteriological methods. PCR has also replaced enzyme immunoassays as a fast and sensitive test for routine diagnostics. Compared to dogs, Bordetella bronchiseptica infections are rare in cats. These can also be detected swiftly and sensitively by PCR.
Since bacterial co-infections are common, it is advisable to also submit a swab with medium for bacteriological testing in order to initiate an appropriate local and/or systemic treatment, especially in cases with ophthalmological changes or in cases of chronic respiratory disease.
As for kennel cough, antibody detection methods are generally less helpful for diagnostics, since many cats will have been vaccinated or will have come into contact with the pathogens as kittens.